Multi-Cancer Gene Panel
All of us have a 1 in 2 lifetime risk of cancer, but some common cancers including breast, melanoma, pancreatic, prostate and ovarian are known to occur more frequently in families, passing from one generation to the next. This is because certain genetic mutations can be inherited.
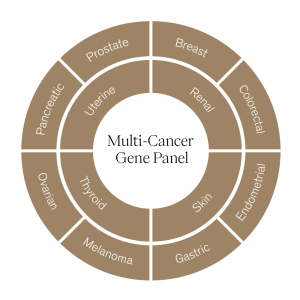
The Multi-Cancer Gene Panel from Everything Genetic analyses seventy-two genes associated with the reported increased risk, in at least one research study, of one or more of the following hereditary cancers: breast, colorectal, endometrial, gastric, melanoma, ovarian, pancreatic, prostate, renal, skin, thyroid and uterine. It is suitable for individuals with a family history of cancer to identify their risk of developing the disease due to an inherited genetic variant.
Why should I consider having this test?
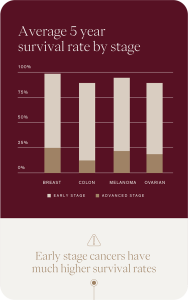
Knowing that you have a genetic mutation enables you to make sure you have the appropriate regular screening and investigations in the future. Many gene mutations are known to be hereditary; if you have a mutation, there is a 50% chance that your siblings and children will have it too.
What does the test involve?
During your consultation on the day of your assessment, your Preventicum Doctor will explain the test and go through some pre-test counselling before you consent to go ahead with it. The test itself is a simple saliva sample that you can do in the clinic on the day of your assessment.
How long does it take to get my results?
Your sample will be sent to the Everything Genetic laboratory in the UK where it will be analysed. Your report will be generated within 4 weeks from the date of your test.
How will I get my results?
Once your genes have been analysed, a personalised results report will be sent to your Preventicum Doctor who will share it with you. If a variant is detected or there is a variant of unknown significance, you will also be contacted by a Consultant Geneticist from Everything Genetic to discuss these results, the implications and next steps. If the results are negative, but you would like to discuss these further, a consultation can be arranged at no additional charge. Discussing your results with a Geneticist and your Preventicum Doctor will help you to:
• understand your risks
• monitor your health
• consider your lifestyle or diet
• protect your family
What will my results show?
There are three possible result outcomes from this test:
• A variant detected result indicates that a fault in one or more of your genes has been found meaning you have an increased risk of developing the cancer related to that gene fault.
• A negative result indicates that the test has not identified any faults or variants that put you at risk of developing the hereditary cancers tested for in the genes analysed.
• A variant of unknown significance (VUS) result indicates that the test has identified a change in the sequence of one or more of your genes, but it is not yet known if that indicates a clinically significant cancer risk. It is unusual to receive a VUS result on any of the genes analysed by this test.
Which diseases are tested?
• Hereditary Breast and Ovarian Cancer (HBOC) – BRCA1, BRCA2 and PALB2
• Other moderate risk breast cancer genes – ATM, CHEK2, BARD1 and NF1
• Other moderate risk HBOC genes – RAD51C and RAD51D
• Other moderate risk ovarian genes – BRIP1
• Li-Fraumeni Syndrome – TP53
• Cowden Syndrome – PTEN
• HNPCC (Lynch Syndrome) – MLH1, MSH2, MSH6, PMS1 and PMS2
• Familial Adenomatous Polyposis (also MUTYH if homozygous) – APC
• Juvenile Polyposis – BMPR1A, SMAD4
• Peutz-Jeghers Syndrome – STK11
• Other bowel cancer genes – POLE and POLD1
• Hereditary diffuse gastric cancer (and lobular breast cancer) – CDH1
• Von Hippel-Lindau – VHL
• Multiple Endocrine Neoplasia – MEN1 and RET
• Gorlin Syndrome – PTCH1
• Paraganglioma predisposition – SDHB and SDHD
• Melanoma genes – CDKN2a, CDK4 and MITF
Which genes are tested?
ABRAXAS1; APC; ATM; AXIN2; BAP1; BARD1; BLM; BMPR1A; BRCA1; BRCA2; BRIP1; CDH1; CDK4; CDKN2A; CHEK2; DICER1; DIS3L2; EPCAM; FANCC; FH; FLCN; GALNT12; HNF1A; HNF1B; HOXB13; KIT; MC1R; MEN1; MET; MITF; MLH1; MLH3; MRE11; MSH2; MSH3; MSH6; MUTYH; NBN; NF1; NTHL1; PALB2; PMS1; PMS2; POLD1; POLE; POT1; PRSS1; PTCH1; PTEN; RAD50; RAD51C; RAD51D; RECQL; RET; RNF43; RPS20; SDHA; SDHAF2; SDHB; SDHC; SDHD; SMAD4; SMARCA4; STK11; TGFBR2; TP53; TSC1; TSC2; VHL; WT1; XRCC2; XRCC3
References:
- Cancer Research UK: Breast Cancer Statistics
- Cancer Research UK: Stomach Cancer Statistics
- Cancer Research UK: Melanoma Skin Cancer Statistics
- Cancer Research UK: Melanoma Skin Cancer Risk
- Cancer Research UK: Pancreatic Cancer Statistics
- Cancer Research UK: Prostate Cancer Statistics
- Cancer Research UK: Prostate Cancer Risk
- Cancer Research UK: Kidney Cancer Statistics
- Cancer Research UK: Thyroid Cancer Statistics
- Cancer Research UK: Risks and Causes of Thyroid Cancer
- Cancer Research UK: Uterine Cancer Risk
- Cancer Research UK: Family History and Inherited Cancer Genes
- World Cancer Research Fund: UK Cancer Statistics
- Bowel Cancer UK: Bowel Cancer
- Target Ovarian Cancer: Ovarian Cancer Risk
- Pancreatic Cancer UK: Hereditary Pancreatic Cancers
- NHS England: Renal Cancer
- Breast Cancer Now: Breast Cancer in Families