View and download full infographic
The term ‘cancer’ strikes fear into the hearts of most people. Unfortunately, it is all too common and overall incidence rates continue to increase. There are approximately 375,000 new cases of cancer per year in the UK and it is estimated that 1 in 2 people in the UK born after 1960 will be diagnosed with some form of cancer during their lifetime. Worryingly, the incidence of under-50s in the developed world being diagnosed with cancer has risen in the past 30 years to the extent that this is considered to be called an ‘epidemic’ by epidemiologists.
Many cancers are preventable, in particular a huge number of cancers are triggered by cigarette smoking which accounts for 15% of all cancer cases. However, many are not, and it is vitally important to find cancers as early as possible because prognosis is dependent upon early detection. In total, 38% of cancers are preventable. There are many types of cancer but cancers in general account for nearly a third (30%) of all deaths in the UK, i.e. 1 in 3 people will die from cancer. At Preventicum, our philosophy is to encourage early detection of potential cancers as well as avoidance of known risk factors.

Risk factors
An individuals’ risk for developing cancer depends on numerous factors which include age, genetics and exposure to risk factors. Lung cancer, bowel cancer, melanoma skin cancer and breast cancer are the most common preventable cancers which account for approximately two-thirds of all preventable cancer cases in the UK. Risk factors include:
-
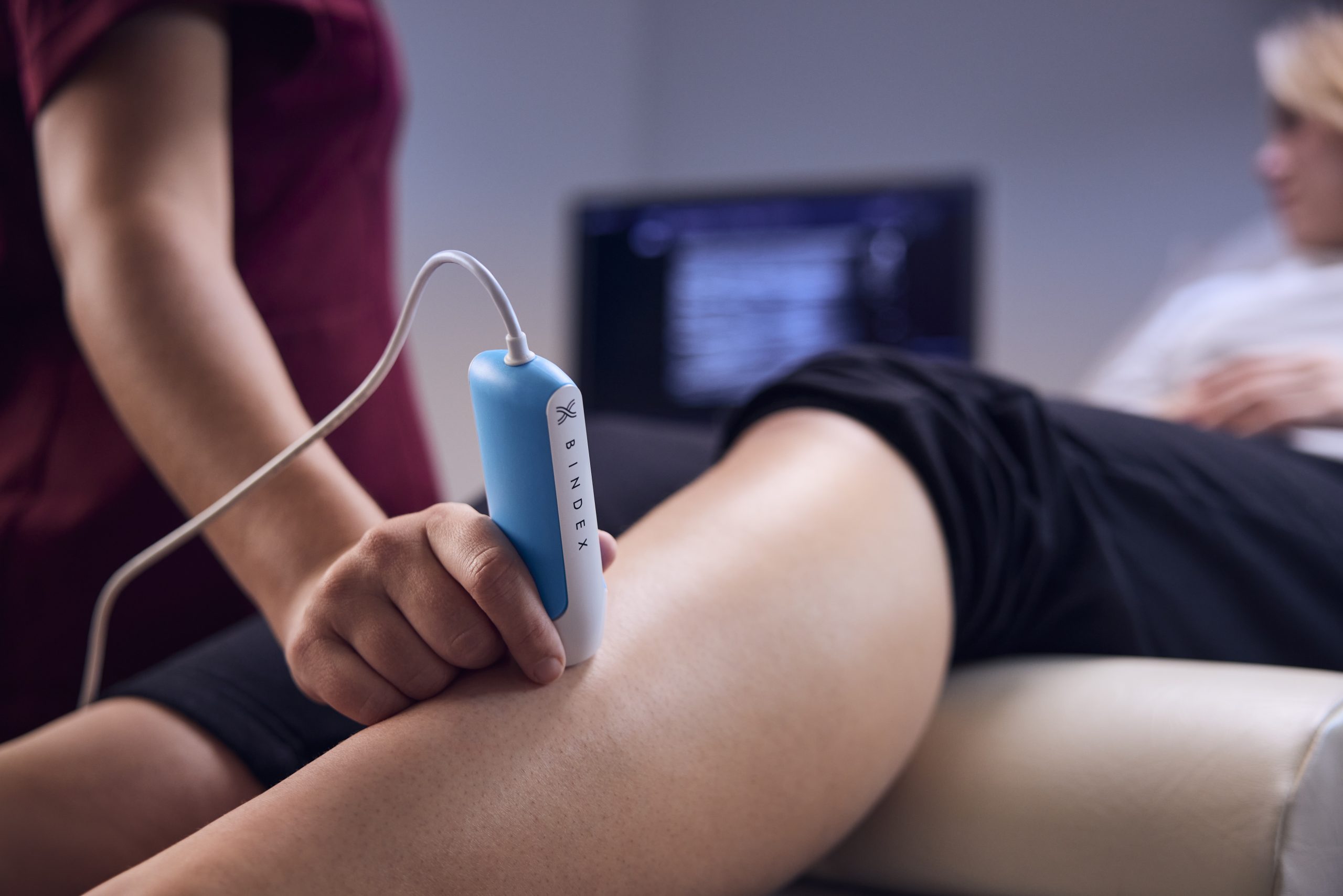
- Smoking is the largest cause of cancer in the UK (15% of all cancer cases).
-
- Obesity and being overweight is the biggest cause after smoking and accounts for 5% of all cancer cases in the UK. Overweight and obesity prevalence has increased in the past 3 decades.
-
- Overexposure to UV radiation, occupational exposure to substances, exposure to specific infections, alcohol and eating too little fibre account for 3-4% of cancer cases.
-
- Exposure to ionising radiation and eating processed meat account for 1-2% of all cancer cases in the UK.
-
- Exposure to air pollution and being sedentary account for 1% or less of all cancer cases in the UK.
Cancer incidence trends in the younger population
The importance of comprehensive medical assessments, especially from a younger age, is becoming more pronounced from recent data which has identified a significant upsurge in cancer diagnoses in the under-50s in developed countries over the past 30 years. Analysis of the G20 group of nations has identified that cancer rates in the 25-29-year-old age range have seen the fastest increase, rising by 22% between 1990 and 2019.
Colorectal cancer has increased by 70% among 15-39-year-olds between 1990-2019. Furthermore, cancer is the leading cause of death for young adults in upper-middle income countries. A recent study published in the journal BMJ Oncology looked at global cases of early onset cancer (cancer in under- 50s) since 1990 and found an increase in cancer diagnoses of nearly 80% and an increase in cancer deaths of 27%.
There have been no definitive explanations for this trend, but this highlights that detailed health screening from a much earlier age is indicated. Research is ongoing into this field and it is predicted that early onset cancer cases will continue to grow for the foreseeable future, despite the trend for the prevalence of smoking to be decreasing. Although genetic factors have a role, the main risk factors that have been identified include diets which are high in red meat and salt, alcohol and tobacco use, physical inactivity, excess weight and high blood sugar.
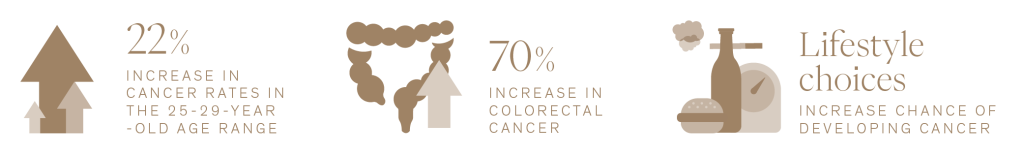
How Preventicum looks for cancer
The findings from these latest research studies and epidemiological data highlights that early detection remains one of our greatest weapons, and that comprehensive, world-class screening including the use of scanning technology is at the forefront. At Preventicum, our advanced Optimal and Ultimate Assessments can help to detect the earliest signs of and risk factors for at least 15 cancers, as well as for heart disease, stroke, diabetes and many other conditions. This is achieved by a combination of information obtained from a detailed Preventicum Doctor consultation, physical examination, blood tests, MRI scans and ultrasound scans.

There has been recent early research into Multi Cancer Early Detection (MCED) tests including the Galleri Test and TruCheck which we are actively monitoring. We continue to appraise the most up to date research into tests which will assist in the diagnosis and prevention of cancers.
Prostate cancer
Prostate cancer is the most common cancer in males in the UK with 52,300 new cases every year (2016-2018). This is 27% of all new cancer cases in males in the UK. Prostate cancer is the 2nd most common cause of cancer death in males in the UK although death rates have decreased by 10% over the past decade. This may be related to advancements in early detection and therapeutic options for treatment.
The most important risk factors for prostate cancer are increasing age and ethnicity. Incidence rates are lower in the Asian ethnic group but increased in the black ethnic group. Family history is also important and prostate cancer risk is over 2 times higher in men whose father has had prostate cancer. The risk increases to approximately 3 times higher in men whose brother has had prostate cancer and is 1.9 times higher in men with a second degree relative who has had the disease. The BRCA 2 gene is closely linked to increased risks of prostate cancer (5 times higher risk for the general population and 7 times higher risk in men under the age of 65). There is no association between BRCA 1 gene and prostate cancer. Our cancer gene test includes detection of BRCA genes alongside another 28 genes which are associated with various cancers.
At Preventicum we offer a prostate health assessment from the age of 45 years which includes a detailed discussion regarding urinary symptoms with your Preventicum Doctor, physical examination of the prostate, PSA blood test and assessing prostate volume on ultrasound and MRI scans. This MRI scan is not a dedicated multi-parametric MRI scan of the prostate, which is a test used by urologists to detect prostate cancer when clinically indicated. These clinical indications include new urinary symptoms, an abnormal prostate examination or an abnormal PSA test, all of which can be identified during our assessments.
We are aware of ongoing research into the use of MRI prostate in screening for prostate cancer and the promising findings. At Preventicum we are actively monitoring this research whilst concurrently ensuring that we continue to offer the most comprehensive packages in preventive healthcare. Following your Preventicum assessment we can help to refer you to a network of recommended urologists for further investigations if appropriate.
Bowel cancer

Bowel cancer is the 4th most common cancer and the 2nd most common cause of death in the UK. Although bowel cancer incidence in younger age groups has increased, overall bowel cancer incidence rates have remained stable over the past 30 years. Mortality rates have decreased by 11% in the last decade, with early identification being one of the key contributors

FAECAL IMMUNOCHEMICAL TEST ( FIT )
The introduction of the FIT, which detects blood in stool, is an important screening test for bowel cancer. This test provides a sensitive and specific non-invasive test for bowel cancer and can guide decisions regarding the clinical need to progress to colonoscopy. At Preventicum the FIT stool test is included in our assessments for all individuals aged over 40 and for those where it is clinically indicated. If a positive result is detected, we can facilitate referrals to a network of colorectal specialists.
Other cancers

Our detailed imaging including MRI and ultrasound scans of the abdomen and pelvis help us to assess the health of organs such as the pancreas, ovaries, uterus, liver, kidneys and bladder so that early changes can be identified and further action can be taken.
Haematological cancers, such as leukaemia and lymphoma, can be difficult to detect due to the non-specific nature of presenting symptoms. However, our combination of a detailed history, thorough physical examination, comprehensive blood tests (especially the full blood count) and imaging tests, which can identify lymph node and spleen changes, can significantly improve the probability of detecting these cancers.

All our assessments include a dedicated thyroid ultrasound to recognise worrying thyroid lesions.

Cervical screening tests can be completed at all assessments, including at times outside of the NHS National Screening Programme, which detect Human Papilloma Virus (HPV), the most important risk factor for cervical cancer.
Testicular cancer incidence rates have increased by 27% since the early 1990s and the highest incidence occurs in males aged 30-34. All male clients are offered a testicular ultrasound to screen for testicular cancer.
References: Cancer Research UK | Institute for Health Metrics and Evaluation (IHME) Zhao J, Xu L, Sun J, et al Global trends in incidence, death, burden and risk factors of early-onset cancer from 1990 to 2019 BMJ Oncology 2023;2:e000049. doi: 10.1136/bmjonc-2023-000049